No products in the cart.



Hormonal Obesity Code
Decoding Hormones Behind Weight Gain
Obesity is not always about calories.
Sometimes, the real trigger lies deeper — within hormonal imbalances that silently disrupt metabolism.
This workshop decodes the hormonal drivers behind weight gain and translates science into practical nutrition strategies.
Hormonal obesity refers to weight gain driven primarily
by endocrine dysregulation rather than excess caloric intake alone.
When hormones are imbalanced, metabolism, appetite, fat storage, and energy expenditure are altered.
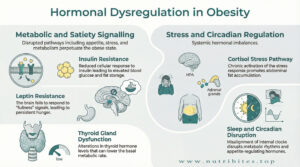
Obesity can result from multiple hormonal imbalances.
Insulin resistance, elevated cortisol, thyroid dysfunction, leptin resistance, and disrupted circadian hormones all play critical roles in weight gain.
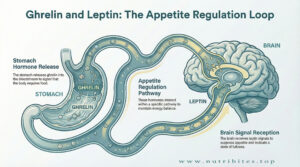
Ghrelin stimulates hunger.
Leptin signals satiety. When leptin resistance develops, appetite remains high despite adequate fat stores.
The hunger-satiety axis becomes dysfunctional.
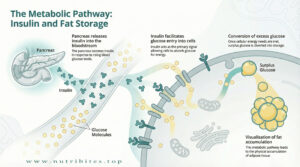
Insulin regulates glucose metabolism.
Chronic elevation leads to increased fat storage and reduced fat oxidation.
Insulin resistance is a cornerstone of hormonal obesity.
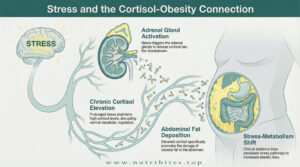
Chronic stress elevates cortisol levels.
High cortisol promotes visceral fat accumulation, increases appetite, and disrupts blood sugar balance.
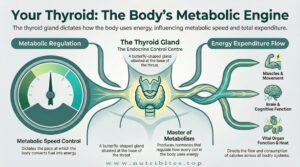
Thyroxine regulates metabolic rate.
Hypothyroidism slows energy expenditure and promotes weight gain even with normal caloric intake.
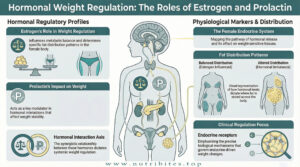
Estrogen influences fat distribution and insulin sensitivity.
Prolactin imbalance may contribute to weight gain through metabolic and appetite-related mechanisms.
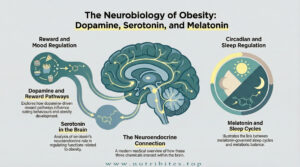
Neurotransmitters influence cravings, mood, and sleep.
Dopamine affects reward pathways. Serotonin regulates mood and appetite. Melatonin controls circadian rhythm and metabolic balance.
Strategic nutrition can support hormonal balance.
Macronutrient timing, fiber intake, protein adequacy, anti-inflammatory foods, and micronutrient optimization all influence endocrine health.
Exercise improves insulin sensitivity,
reduces cortisol, supports dopamine balance, and enhances metabolic flexibility.
Intensity, duration, and type matter.
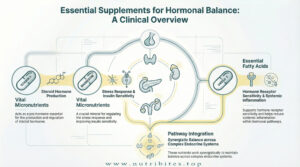
Evidence-based supplements may support hormonal balance
when properly indicated. Magnesium, vitamin D, omega-3 fatty acids, adaptogens,
and targeted micronutrients can enhance outcomes.
Hormonal obesity requires precision, not restriction.
Decode the hormones. Design targeted interventions. Transform patient outcomes.
The Hormonal Obesity Code is an intensive 2-day scientific workshop designed to help nutrition professionals deeply understand the hormonal mechanisms behind weight dysregulation. This program provides an evidence-based approach to evaluating and managing hormonal imbalances linked to obesity, metabolic disorders, and endocrine dysfunctions.
During the workshop, you will explore the physiology of key hormones such as insulin, leptin, ghrelin, cortisol, thyroid hormones, estrogen, prolactin, dopamine, serotonin, and melatonin — and understand how disruptions in these pathways contribute to weight gain, fatigue, cravings, low metabolic rate, and adiposity.
Through structured learning and real clinical insights, you will gain practical tools to assess hormonal patterns, interpret symptoms of imbalance, and build nutrition strategies tailored to each patient’s metabolic and endocrine profile.
This workshop is taught by Dr. Heba Samir, Consultant of Internal Medicine & Clinical Nutrition, with extensive experience in endocrine-related obesity and metabolic conditions.
محتوى الدورة
Day 1
-
الفيديو 1
-
الفيديو 2
-
video 3
-
video 4
-
video 5
-
video 6
-
video 7
Day 2
احصل على شهادة
أضف هذه الشهادة إلى سيرتك الذاتية لإبراز مهاراتك وزيادة فرصك في لفت الانتباه.